Every NJ payer. Every rule. Pre-loaded.
Every major NJ ABA payer pre-configured. CPT limits, required documents, submission formats, diagnosis codes — all current, all enforced automatically.
- 6
- NJ payers configured
- 59
- Enforced rules
- 0
- Manual payer lookups
Horizon BCBS NJ
CommercialSubmission
Phone
Initial
6 months
Re-Auth
6 months
- Caregiver plan required
- Discharge & fading plan
- Standardized assessment (2+ tools)
- BCBA billing required
Horizon NJ Health
MCOSubmission
Phone
Initial
6 months
Re-Auth
6 months
No fax — phone submission only
- 799.0–799.9 accepted
- BCBA supervision required
- Daily visit caps enforced
Aetna NJ
CommercialSubmission
Fax
Initial
3 months
Re-Auth
6 months
3-month initial auth (shorter than most)
- Fax PA packet PDF
- Assessment within 12mo
- BCBA billing required
AmeriHealth NJ
CommercialSubmission
Fax
Initial
6 months
Re-Auth
6 months
- Diagnosis enforcement
- BCBA billing required
UHC Community Plan NJ
MCOSubmission
Phone
Initial
6 months
Re-Auth
6 months
- Managed Medicaid plan
- Standard CPT coverage
NJ Medicaid FFS
MedicaidSubmission
Portal
Initial
No PA (initial)
Re-Auth
PA required
No PA required for initial — re-auth only
- ASD diagnosis from a qualified provider required
- Covers through age 21
- Fee-for-service plan
Question about a specific payer? hello@korafy.ioAdditional payers added on request. FHIR-based submission available January 2027 (CMS mandate).
Every payer rule, enforced before submission.
Red “hard stop” badges block submissions that would be rejected. Your team only sees what passes the rules.
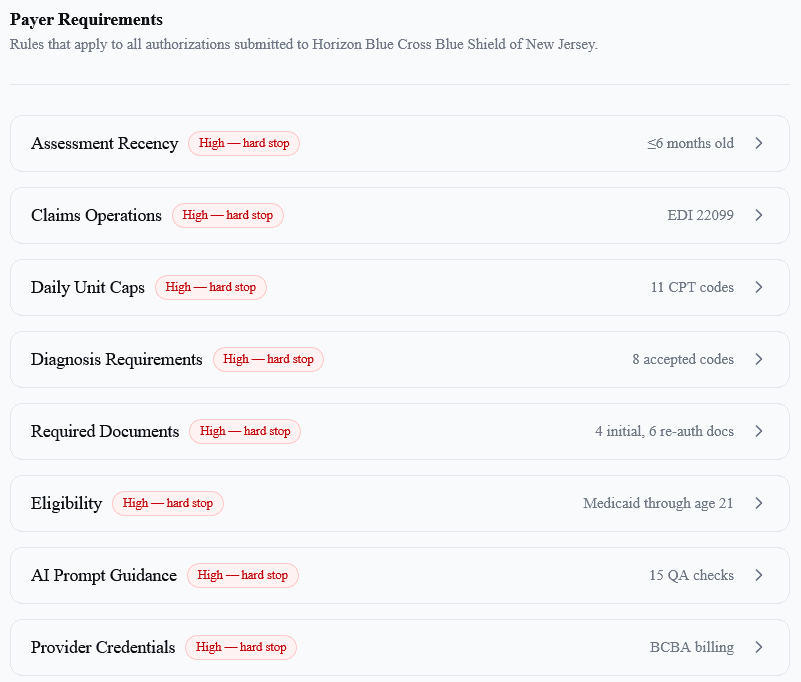
Payer requirements configuration — Horizon BCBS NJ
Ready to stop chasing payer rules?
Be among the first NJ ABA practices on Korafy.